When Local Improvement Wasn't Enough: How St. Clair Hospital Scaled a Lean Culture
May 29, 2026CASE STUDY
How St. Clair Hospital scaled a Lean culture across 2,400 employees with a two-person improvement team
At a glance
- 328-bed...
What 200,000+ Frontline Ideas Look Like When Leaders Actually Listen
April 3, 2026This blog summarizes key insights from a comprehensive whitepaper detailing UMass Memorial Health's remarkable transformation journey.
...
8 Wastes of Lean: Examples You'll Recognize From Your Job
March 25, 2026Every process in every organization contains waste. That claim sounds dramatic until you start looking for it. Then it becomes obvious.
...
How Continuous Improvement Powers Operational Excellence in Healthcare
March 6, 2025Healthcare leaders are increasingly striving to embed the principles of operational excellence and continuous improvement in their...
Operational Excellence in Healthcare: How to Build a Culture of Continuous Improvement
August 12, 2024According to a study by McKinsey & Company, hospitals in the United States could save $130 billion annually by improving their operational...
How Transformation in Healthcare Can Help Improve Operational Decisions
April 3, 2026Transformation in healthcare involves integrating technology to improve patient care, streamline administrative processes, and enhance...
Mark Graban & Greg Jacobson Discuss Continuous Improvement and Customer Experience Design
October 31, 2023Join Greg Jacobson, MD, co-founder and CEO of KaiNexus, and me for another episode of the KaiNexus Continuous Improvement podcast.
Tiered Huddles: How Structured Daily Communication Drives Improvement
April 3, 2026Most organizations have meetings. What they lack is a system that connects what happens on the front lines to what leadership needs to know...
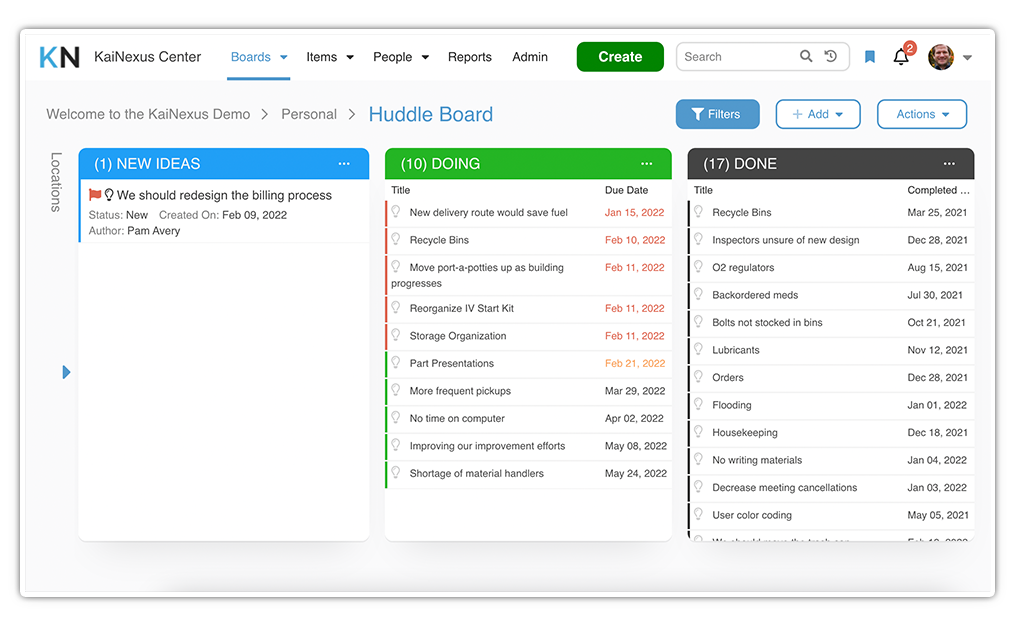
Huddle Boards: How Healthcare Teams Use Them for Process Improvement
April 3, 2026In sports, a huddle happens when the team gathers to strategize before a play. Everyone learns their role, the plan is confirmed, and the...